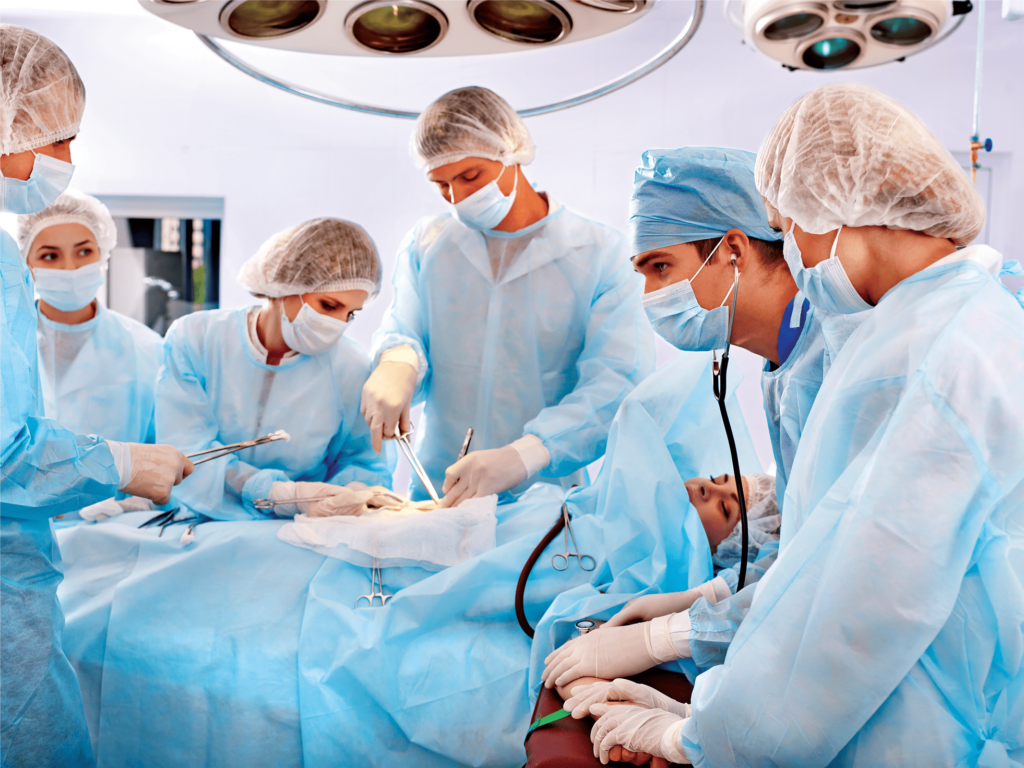
Standard infection control practices are carried out in every hospital. Despite hospitals best efforts to minimize the infection rates, healthcare workers such as doctors, surgeons, dentists, clinical officers, and nurses are still contracting infections and diseases while dealing with the patients, resulting in increased cross-contamination rate among hospital staff. Moreover, hospital co-workers are more liable at spreading infections through direct contact and indirect contact with inanimate and animate objects.
Health-care Associated Infections (HAIs) have become increased concern both in the developed and developing countries. Healthcare-acquired infections (HAIs), also known as nosocomial infections, are infections that patients get while receiving treatment for medical or surgical conditions. HAIs occur in all settings of care, including hospitals, surgical centers, ambulatory clinics, and long-term care facilities such as nursing homes and rehabilitation facilities.
According to WHO (2013) report, in developing countries where the HAIs prevalence is from 25-40%, these infections pose a major threat. Further studies indicate that HAIs have a major impact on poor countries as they have limited resources such as HAIs imposes an extra strain on patients, families, health-care set-ups, resulting in increased morbidity and mortality that eventually leads to the increasing healthcare cost. One study estimated that annually 1.4 million people globally suffer from infections acquired in hospitals.
Moreover, the increased nosocomial/HAIs have escalated the problem of antibiotic resistance. Studies carried out have shown that 37% of the nosocomial infections in ICUs are due to the increased antibiotic resistance among microorganisms that contribute to the increase cross-contamination among patients and co-workers.
To prevent and control the HAIs spread better means need to be figured out, such as providing reliable healthcare solutions. One solution includes the introduction of Protector® Antimicrobial Disposable Range in Healthcare set-ups. Following are the complete disposable products range that can help control the HAIs spread.
Disposable Gloves:
 Gloves are the foremost part of Personal Protection Equipment (PPE) protocol. Wearing gloves in healthcare set-up enhances personal safety against when exposed to body fluids. Gloves are used to avoid cross contaminations among patients, objects, and the environment. Therefore, gloves are recommended during clinical practices.
Gloves are the foremost part of Personal Protection Equipment (PPE) protocol. Wearing gloves in healthcare set-up enhances personal safety against when exposed to body fluids. Gloves are used to avoid cross contaminations among patients, objects, and the environment. Therefore, gloves are recommended during clinical practices.
However, ordinary disposable gloves get easily contaminated and pathogenic Staphylococcus species have been reported as the most predominant microorganisms present on procedure gloves and their boxes. Studies were carried out and samples were collected from glove boxes and it was evaluated that nine out of ten gloves were contaminated with bacteria, among them species coagulase-negative Staphylococcus (CNS) species was the most recurrent. These microorganisms cause significant contamination and infectious spread with increased HAIs in hospital set-ups.
Protector® Antimicrobial Gloves kill effectively most virulent microorganisms upon contact and prevent the growth of these microorganisms by 99.99%. Protector® Antimicrobial gloves are highly recommended in Intensive Care Units, Surgical Sites and Critical Areas where HAIs needed to be controlled and minimized for patient’s safety.
Disposable Isolation Gowns:
 Gowns are the second most important PPE after gloves in the healthcare settings. Isolation gowns are defined by Association for the Advancement of Medical Instrumentation (AAMI) as the protective attire used to safeguard both health care workers and patients from the microbial contaminations, infections and body fluids in patient isolation situation. The Food and Drug Administration (FDA) states that: “a gown is intended to protect healthcare personnel and patients from the transfer of microorganisms, body fluids, and particulate materials”. Isolation gowns act as a physical barrier against the transfer of microorganisms and other biological matter.
Gowns are the second most important PPE after gloves in the healthcare settings. Isolation gowns are defined by Association for the Advancement of Medical Instrumentation (AAMI) as the protective attire used to safeguard both health care workers and patients from the microbial contaminations, infections and body fluids in patient isolation situation. The Food and Drug Administration (FDA) states that: “a gown is intended to protect healthcare personnel and patients from the transfer of microorganisms, body fluids, and particulate materials”. Isolation gowns act as a physical barrier against the transfer of microorganisms and other biological matter.
However, ordinary isolations gowns are useless against most virulent microorganisms found in blood, body fluids, and other potentially infectious materials (OPIM) of patients. Therefore, there is a need to interrupt the transmission cycle and protect susceptible patients from getting infected over and over. Protector® Antimicrobial Isolation Gowns are effective against most of these virulent microorganisms, providing maximum protection to the patients and has 99.99% efficacy against these microorganisms.
Disposable Surgical Gowns:
Similarly, surgical interventions or contaminations are associated with risk of postoperative wound infections for patients and catching of infections for surgeon themselves. As a result, every effort is made by the surgeons and operating room staff to adhere to proper sterile techniques goes in vain and the surgical-site infections are the threat for both the surgeons and the patients.
Protector® Antimicrobial Surgical Gowns have built-in antimicrobial properties that kill any microorganisms that come in contact. The antimicrobial surgical gowns give maximum protection to the surgeons and then ultimately to the patients. Both standard and reinforced gowns are available.
Disposable Caps:
 Microbial contamination can occur during surgeries in the operating rooms leading to serious and sometimes life-threatening postsurgical complications. Postsurgical complications include severe infections, inflammations, delays in healing, wound dehiscence, and trauma. Literature reports that the operating staff and hospital co-workers shed a large number of microorganisms during working. These microorganisms are usually associated with the skin particles residing on different parts of the human body.
Microbial contamination can occur during surgeries in the operating rooms leading to serious and sometimes life-threatening postsurgical complications. Postsurgical complications include severe infections, inflammations, delays in healing, wound dehiscence, and trauma. Literature reports that the operating staff and hospital co-workers shed a large number of microorganisms during working. These microorganisms are usually associated with the skin particles residing on different parts of the human body.
Different published reviews suggest the dissemination and transmission of these pathogens occur from the head and neck regions of surgeons and co-workers. Further literature cites that the common flora that colonizes the human skin and mucosa include Gram-positive cocci (Staphylococcus sp., Streptococcus sp., Moraxella sp.), Gram-negative rods (including anaerobes) and among them most are pathogenic residing as opportunistic microorganisms.
To avoid the cross contaminations in the intensive care units, operating rooms and postoperative care units, it is necessary to implement the use of disposable caps and practice standard protocols. Maintaining a high level of cleanliness and following proper protocol is necessary for both the surgeons, healthcare workers, and patients. Even with the advancement in technology, the Surgical Site Infections (SSIs) are still at increasing rate as microorganisms are developing resistance, turning out particularly dangerous for patients during surgeries.

Surgical site infections (SSIs) can be resolved by surgeons wearing Protector® Antimicrobial Doctor Caps during surgeries. While the problem with pathogenic dissemination in the hospital environment can be controlled with the use of Protector® Antimicrobial Mob Caps by other healthcare workers during general working. This will reduce the microbial aggregations and epidermal bioburden on healthcare set-ups, providing maximum protection to surgeons, healthcare workers, and patients.
Disposable Facemasks:
 Air-borne diseases are affecting a major part of a population. The modern urban lifestyle and rapidly growing industries have polluted the environment. Air-pollution (smoke, smog, haze, and allergens) is a major threat to human health living in busy urban areas where they are continuously exposed to toxic elements and small particulate matters contributing to widespread chronic respiratory diseases and heart diseases. Expansion of infrastructure and transport systems have made situations more critical.
Air-borne diseases are affecting a major part of a population. The modern urban lifestyle and rapidly growing industries have polluted the environment. Air-pollution (smoke, smog, haze, and allergens) is a major threat to human health living in busy urban areas where they are continuously exposed to toxic elements and small particulate matters contributing to widespread chronic respiratory diseases and heart diseases. Expansion of infrastructure and transport systems have made situations more critical.
Moreover, Hospital Acquired infections (HAIs) is increasing rapidly and has globally become a major concern for healthcare set-ups. In a hospital environment, airborne infections spread when bacteria or viruses travel through dust particles or small respiratory droplets that become aerosolized when an infected person sneezes or coughs. These infections can spread through both opportunistic and pathogenic microorganisms present in healthcare setups and can easily be transmitted to doctors, healthcare workers, patients, and visitors. One of the cause is the cross-contamination of microorganisms that are responsible for the transmission of infections.
Protector ® Antimicrobial Facemasks provide maximum protection against microorganisms, viruses, allergens, smoke, haze, and fine particles. It prevents the air-borne transmission when an environment is highly contaminated with bacteria and other microorganisms on the roads, industrial manufacturing, healthcare set-ups, and pathological labs or in culinary industries. Microorganisms are everywhere and in order to protect against the deadly diseases, the Protector® Antimicrobial Facemask is the best option for maximum protection.
Disposable Lab Coats:
 White coats are worn as personal protection; however, there has been a rising concern over lab coats in disseminating the pathogenic microorganisms in hospital settings. Literature reviews are available that states lab coats to be potentially contaminated with pathogenic drug-resistant bacteria. One reason for lab coats contamination may be the continuous shedding of bacteria from patients that then spread in the hospital environment. Other studies conducted states that the patient’s skin can also be a source of contamination for the health care workers’ white coats.
White coats are worn as personal protection; however, there has been a rising concern over lab coats in disseminating the pathogenic microorganisms in hospital settings. Literature reviews are available that states lab coats to be potentially contaminated with pathogenic drug-resistant bacteria. One reason for lab coats contamination may be the continuous shedding of bacteria from patients that then spread in the hospital environment. Other studies conducted states that the patient’s skin can also be a source of contamination for the health care workers’ white coats.
Despite hospitals best effort to minimize the threat for HAIs, healthcare workers contaminated lab coats serve as potential vectors of disease, disseminating virulent microorganisms among patients. Health care workers and patients are at greater risk of contracting infections and diseases.
Protector® Antimicrobial Lab Coats with built-in antimicrobial features will kill any microorganisms that it contracts. The Antimicrobial Lab Coats are effective against wide range of microorganisms and help to control the horizontal transmission of bacterial and other microbial contamination.
Disposable Bed and Pillow Covers:
 During the patients’ course of stay at hospitals, most of the time is spent resting on the hospital beds. Therefore, patients are in continuous contact with room appurtenance especially bed and pillow cover. The prolong stay can lead to acquiring of Health Acquired Infections (HAIs); contamination through patient’s direct contact has been identified as a possible route. Hospitals follow strict protocols to maintain hygiene and cleanliness this include washing, disinfecting and sterilizing bed linens. However, as soon as bed linens are exposed to the patient, microorganisms start to settle and multiply exponentially on the linen surface.
During the patients’ course of stay at hospitals, most of the time is spent resting on the hospital beds. Therefore, patients are in continuous contact with room appurtenance especially bed and pillow cover. The prolong stay can lead to acquiring of Health Acquired Infections (HAIs); contamination through patient’s direct contact has been identified as a possible route. Hospitals follow strict protocols to maintain hygiene and cleanliness this include washing, disinfecting and sterilizing bed linens. However, as soon as bed linens are exposed to the patient, microorganisms start to settle and multiply exponentially on the linen surface.
Current standards for cleaning and disinfectants are inefficient to subsidize hospital infections and diseases. Housekeeping and launders of hospitals wash, disinfects and in some cases sterilize the bed and pillow covers with prescribed protocols. The use of disinfectants such as hypochlorite, hydrogen peroxide, or other agents to reduce bioburden is also not effective against drug-resistant microorganisms such as MRSA. Thus, the lack of hygienic solutions and commitment by hospitals are turning most hospital beds into deathbeds.
We need serious solutions for the addressed problems. Protector® Antimicrobial disposable bed and pillow covers with built-in antimicrobial properties are the best choices to fight against the deadly microorganisms. Microbes are killed upon contact with the surface of bed and pillow covers. Antimicrobial bed and pillow covers not only provide protection against microorganisms but also help us save water and operating cost including washing, disinfecting, and sterilization hence a convenient and reliable solution.
Disposable Shoe Covers:
 Shoe Covers are primarily worn in operating rooms to protect the wearer from the contaminations such as blood and other body fluid may be released when patients undergo surgical procedures. Literature review confirms the survival of microorganisms for weeks on inanimate objects. And thus shoe covers act as a vehicle for nosocomial infection in the theatre.
Shoe Covers are primarily worn in operating rooms to protect the wearer from the contaminations such as blood and other body fluid may be released when patients undergo surgical procedures. Literature review confirms the survival of microorganisms for weeks on inanimate objects. And thus shoe covers act as a vehicle for nosocomial infection in the theatre.
The delicate surgeries make shoe covers to be necessarily worn in operation theaters, ICUs, CCUs, and NICUs where patients are critically ill and need to be given extra care. In surgeries such as hip arthroplasty or open heart surgery, where air-borne contamination can become a possible route for nosocomial infections and may put the life of the patient at risk.
Protector® Antimicrobial Shoe Covers with built-in antimicrobial features kills the microorganisms that come in contact with the shoe cover, preventing the dispersal of airborne microorganisms. Thus, limiting the rate of Health Associated Infections (HAIs) healthcare set-ups.
Disposable Waste Bags:
 Health Associated Infections (HAIs) are most problematic for the developing countries. Improper management and handling of the waste counts for major HAIs spread. Hospital wastes include any solid, fluid or liquid materials. The waste may be generated during short term or long term observational, diagnostic, therapeutic and rehabilitative services.
Health Associated Infections (HAIs) are most problematic for the developing countries. Improper management and handling of the waste counts for major HAIs spread. Hospital wastes include any solid, fluid or liquid materials. The waste may be generated during short term or long term observational, diagnostic, therapeutic and rehabilitative services.
With a growing population, a greater number of healthcare institutions are built that every day generates a voluminous amount of waste. These wastes are generated by the hospital, nursing homes, and other healthcare institutions. Hospital waste includes garbage, rubbish, and biomedical waste. The types include body parts, organs, tissues, blood and body fluids along with soiled linen, cotton, bandage, and plaster casts. Other waste may consist of infected or contaminated objects such as medical supplies, syringes, scalpels and lancets, and glass from broken equipment. These material contains pathogens in immense number. These material contains pathogens in immense number.
 To avoid any disease breakout either endemic, sporadic or epidemic from these wastes, it is necessary to maintain hygienic, aesthetic, clean, and controlled conditions at healthcare set-ups. Protector® Antimicrobial Waste Bags with antimicrobial features prevent microbial escape into the environment. Protector® General Waste Bag and High-Risk Bag help in proper management of waste. These measures allow proper collection, segregation, storage, transportation and treatment of waste in a safer manner to prevent nosocomial or Hospital Associated Infections (HAIs).
To avoid any disease breakout either endemic, sporadic or epidemic from these wastes, it is necessary to maintain hygienic, aesthetic, clean, and controlled conditions at healthcare set-ups. Protector® Antimicrobial Waste Bags with antimicrobial features prevent microbial escape into the environment. Protector® General Waste Bag and High-Risk Bag help in proper management of waste. These measures allow proper collection, segregation, storage, transportation and treatment of waste in a safer manner to prevent nosocomial or Hospital Associated Infections (HAIs).