During the patients’ course of stay at hospitals, most of the time is spent resting on the hospital beds. Therefore, patients are in continuous contact with room appurtenance especially bed and pillow cover. The prolong stay can lead to acquiring of Health Acquired Infections (HAIs); contamination through patient’s direct contact has been identified as a possible route. Hospitals follow strict protocols to maintain hygiene and cleanliness this include washing, disinfecting and sterilizing bed linens. However, as soon as bed linens are exposed to the patient, microorganisms start to settle and multiply exponentially on the linen surface.
Infected patient resting on the bed acts as a source of the microbial contamination due to continuous shedding of skin & hair, saliva, and sebaceous particles from their body along with pathogens and within no time they start accumulating in bed linens. Bedcovers are generally replaced once a day providing adequate time for microbial buildup increasing the risk of HAIs among patients, healthcare workers and visitors. Even if they are washed, disinfected and sterilized with proper protocol many multidrug resistant organisms remain on the surface of bed and pillow covers.
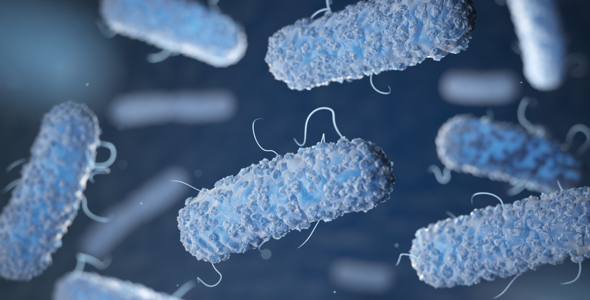
MRSA, VRE, E. coli, Providencia and Klebsiella species are most commonly found on patient beds & contaminated surfaces and are easily cross contaminated. The work carried out by different scientist’s states that VRE strains can subsist for 11 weeks on bed linen even after proper disinfection. The prolong survival on inanimate surface such as linens makes them resistant to most disinfectants and increasing the nosocomial transmission frequency of VRE.
The possibility to get infected becomes six times higher for the next patient using the same bed if the bed & pillow covers are contaminated. According to American journal of Infection Control (IC), if the patient occupying bed before was on antibiotics, the next patient of getting C.difficile infection goes up by 22%. Another study by Columbia University Medical Center (CUMC) indicated 38% patients’ bed pillows are contaminated by more than three different types of virulent microorganisms including Klebsiella, Pseudomonas, and Clostridium.
York university research claims every year at least 29,000 patients are dying by C.difficile alone. So how these microorganisms really carry out its action such effectively?
For instance, patient on antibiotics for C.difficile continuously shed germs cells from their gastrointestinal tract that can be easily transmitted to the nearby furniture and surfaces such as mattress, bed side tables and bedframes. These microorganisms grow exponentially and meanwhile wait patiently for their next victim admitted on the same bed.
Bed and pillow cover also get contaminated through talking, sneezing, and coughing, excretions such as body fluids, urine, and blood spills. Indoor microorganisms already present in healthcare facility also participates in the disease spread and infections. The continuous prevalence and genetic evolvement of microorganisms with time makes them drug resistant that makes it even a bigger challenge for the hospital staff to control infectious spread.
In another research, 200 samples of hospital linen were collected, and the most abundant microorganisms were of human source (coagulase-negative staphylococci) and of environmental source (Bacillus spp., moulds). It concluded that these contaminated bed linens can advance into vectors for pathogenic transmission or even pathogens residing on linen may become airborne during bed-making and possibly contaminate other surfaces. Other than these microorganisms Acinetobacter baumannii was found on bed linen and curtains, and resistant strain such as MRSA was found also found on uniforms worn by health workers and on bed linen.
Current standards for cleaning and disinfectants are insufficient to subsidize the hospital infections and diseases. Housekeeping and launders of hospitals wash, disinfects and in some cases sterilize the bed and pillow covers with prescribed protocols. The use of disinfectant such as hypochlorite, hydrogen peroxide, or other agents to reduce bio burden is also not effective against drug resistant microorganisms such as MRSA. Thus, the lack of hygienic solutions and commitment by hospitals are turning most hospital beds into deathbeds.
Patients’ Bedcovers: cradle of deadly microorganisms Patients spend most time resting during their treatment at hospitals and in that time period they come into contact with various pathogenic microorganisms. Moreover, these patients are in continuous taction with room accessories especially bed and pillow cover that possibly can act as cause for infectious spread. These bed and pillow covers can get contaminated by patients’ secretions, body fluids, and blood which have plenty of microflora spreading the Hospital Acquired Infections (HAIs).
We need serious solutions for the addressed problems. Protector® Antimicrobial disposable bed and pillow covers with built-in antimicrobial properties are the best choice to fight against the deadly microorganisms. Microbes are killed upon contact with the surface of bed and pillow covers in three-steps process.
- Rupturing the microorganism’s cell wall
- Denaturing enzymes and vital molecules of microorganisms
- Destroying the DNA to stop replication of microorganisms
Protector® enables us to prevent microbial growth & buildup and has 99.99% effective against various microorganisms and conforms to ISO 22196, and ASTM E 2180 for its antimicrobial performance. Protector® Antimicrobial bed and pillow covers not only provide protection against microorganisms but also help us save water and operating cost including washing, disinfecting, and sterilization hence a convenient and reliable solution.